Pancreatic Surgery
By
Dr.Bipin Vibhute
What is a Pancreatic Surgery?
When your doctor declares that you need pancreatic surgery, take the matter seriously. Often overlooked, pancreas as an organ is indispensable what with it being responsible for breaking down the nutrients in our food and transporting them throughout the body or for creating the hormone, insulin.
Pancreatic surgery is required when someone has problems with their pancreas such as pancreatic cancer or pancreatitis (inflammation and auto-digestion of the pancreas). To contextualize, auto-digestion refers to the process in which the enzyme responsible for helping break down the nutrients of the food consumed destroys its tissue.
Pancreatic Surgery Guide
Skim through this Pancreatic surgery guide that covers every important aspect of this disease, its causes, symptoms and Treatments.
1. Who is eligible for pancreas surgery?
You must know all the conditions that will justify a pancreatic surgery. The silver lining is that not ALL pancreatic abnormalities will require surgery.
Here they are so to keep you in the know:
1. PANCREATIC CYSTS –
Some may even turn cancerous, if not treated at the right time.
2. ACUTE PANCREATITIS –
A single attack involving bleeding, swelling and damage to the pancreas and its blood vessels after inflammation and auto digestion after which the organ may return to normal.
3. CHRONIC PANCREATITIS –
Inflammation and auto digestion of the pancreas which does not subside and becomes worse over time. This disease hits people who are between the ages of 30 to 40.
4. PANCREATIC NEUROENDOCRINE CANCER –
A rare type of cancer which rises from the hormone-secreting cells.
2. Who might need pancreas surgery?
We will be discussing two diseases here, which may require you to have a pancreas surgery done. Their symptoms will also be mentioned so that you will know what to look out for.
i. PANCREATITIS –
Symptoms of this disease tend to occur suddenly. They are:
● Abdominal pain
● Difficulty in eating
● Weight loss
● Diarrhea
● New-onset diabetes (occasionally)
ii. PANCREATIC CANCER –
Symptoms of this disease tend to occur gradually, taking days, weeks or even months. They are:
● Weight loss
● Diarrhea
● New-onset diabetes
● Jaundice (yellowing of the skin and eyes) sans the pain
● Dark urine and gray stools
3. How is pancreas surgery performed?
A pancreas surgery will be performed depending on the disease that a person is suffering from.
We sympathize with all readers who happen to be either a prospective patient or their family member. While the impending surgery can be daunting, some of it may also be laced by curiosity. Therefore, this segment of the blog will aim to explain how pancreas surgery is conducted.
Some of the surgical procedures that have been considered safe and effective are as follows:
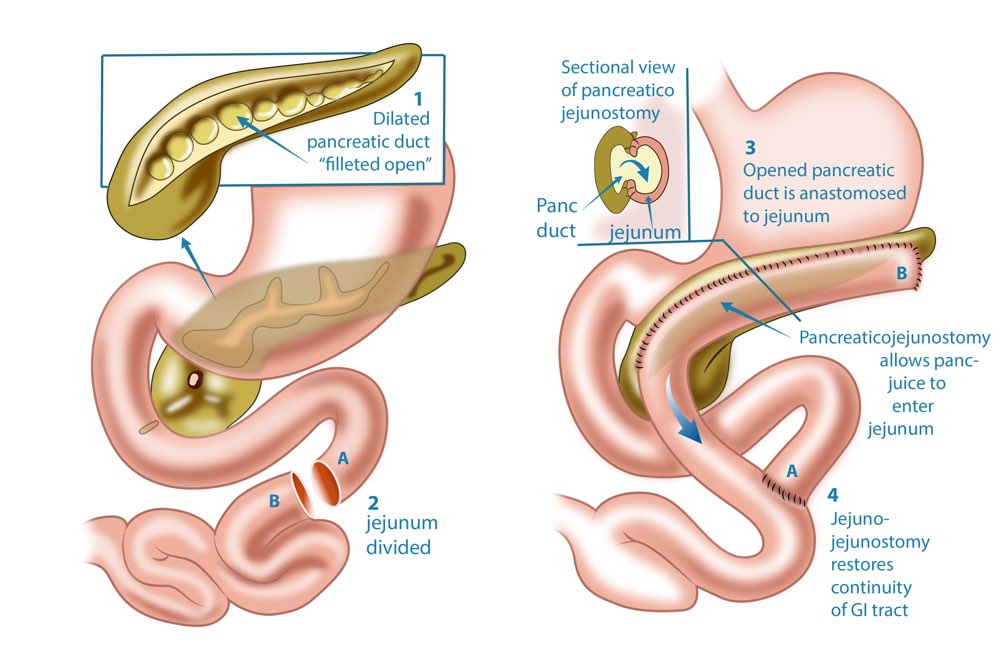
i. The Whipple Procedure –
Also known as pancreaticoduodenectomy, this procedure works best for patients suffering from pancreatic cancer or some other benign complications restricted to the head of the pancreas.
The surgeon will remove the head of the pancreas, part of the bile duct and the gall bladder. They will then reconnect the remaining pancreas to the intestine, bile duct and stomach.
ii. Distal pancreatectomy –
This surgical procedure will often be laparoscopic meaning it will be aided by a small camera and smaller incisions at the surgical site.
This procedure intends to remove tumors at the end or tail of the pancreas.
iii. Total pancreatectomy –
A relatively rare procedure because of the undisputable side-effects attached to it such as diabetes, this surgery constitutes removal of the entire pancreas, the gallbladder, part of the stomach, small intestine and the spleen. It is performed when cancer spreads throughout the pancreas but can still be removed.
iv. Endoscopic retrograde cholangiopancreatography –
ERCP is performed when the cause of pancreatitis seems to be something such as a gallstone lodged in the bile duct. In this procedure, a tube with a tiny video camera at the end of it will be slid down the throat into the small intestine and stomach after which dye will be injected into the drainage tube of the pancreas to locate the possible obstruction.
The purpose of the dye is to produce enhanced images of the pancreas and the bile ducts on the X-ray machine. This helps the doctor view the site of the blockage after which he or she can remove the hindrance. Special instruments such as a balloon catheter or a basket catheter are inserted through the tube to remove this obstruction or stretch a segment of the bile duct.
v. Pancreatic pseudocyst drainage –
A pancreatic pseduocyst is caused due to chronic pancreatitis. This is a fluid-filled sac that forms in the abdomen and is comprised of pancreatic enzymes, blood, and necrotic (dead) tissue.
To remove it, endoscopic drainage is required in which the fluid is removed from the pseduocyst. The process of inserting a tube is the same: it is inserted just as it is in ERCP except the dye is replaced with surgical tools that are positioned on the tube to drain the fluid all while looking at the video footage of the organs concerned.
vi. Bypass surgery –
This procedure is carried out for unblocking a blocked bile duct in which the flow of bile will be rerouted to the small intestine instead of the common bile duct, bypassing the pancreas. This surgery can be a laparoscopic one, thus making it minimally-invasive.
vii. Spleen surgery –
When pancreatic cancer starts affecting the splenic artery or the lymph nodes in the hilum of the spleen, it is best to remove the spleen all while carrying out a distal pancreatectomy.
viii. Stent surgery –
This surgery is carried out to treat the symptoms of pancreatic cancer. A stent may end up causing more problems rather than solving them. Some of its complications include the stent getting blocked due to bile-build up or cancer growing through it, infection in the stent or the stent moving out of its original place.
Types of stent surgeries include:
a. Duodenal stent: When pancreatic cancer starts to block the first part of your intestine, a stunt will be installed to keep the duodenum open. This should help significantly.
b. Bilary stent: When pancreatic cancer starts to block your bile duct and causes intense jaundice, a stent will be installed in your bile duct.
While intriguing, one must not overlook the fact that such surgical procedures should only be performed by surgeons who have more than enough experience in this field. Pancreas surgeries require precision and focus while operating as pancreas is a tricky organ to reach into.
Our suggestion will always be to approach surgeons who know their way extremely well around the human pancreas and the areas surrounding it.
4. What happens after surgery?
The aftermath is neither suspenseful nor anticlimactic. This is because the post-pancreatic surgery experience can be obviously hard to come to terms with.
There’s no denying it that it is a major operation and major operations will also involve risks and complications.
Complications after pancreatic surgery such as the leakage of pancreatic juices from the incision and drastic changes to your digestive system are to be expected.
An aspect to focus more on is that such procedures will extend your life span and make you healthier. This is the thought which a patient and their family should focus on when the former awakens after the surgery.
A fact that most people might not be aware of is that if a patient is diagnosed with diabetes before a pancreatic surgery, their blood sugar levels will improve and stabilize more than ever after the operation!
Be prepared to be kept in the hospital for a considerable amount of time so that you can recover under expert guidance. You may also develop weakness or temporary diarrhea after surgery.
5. Cost of pancreatic surgery
In India, the cost of pancreatic surgery could range from Rs. 3.5 Lakh to Rs. 6 Lakh.
Of course, when it is a matter of which pancreatic disease is to be treated, the cost may fluctuate or deflate.
When planning out your finances, make sure that you add in consultation fees, medication, accommodation, the cost of commute to and from the hospital, etc.
Many hospitals and medical centers in metropolitan cities such as Mumbai and Delhi offer exemplary hospital treatment and surgeries that can be applauded for their results.
Such a big surgery may be costly but one must think of the result: a new and healthy life.
6. Care after pancreatic surgery
Obviously, care after such a tremendously challenging surgery is necessary.
And, feeling weary after the surgery and experiencing pain while recovering at home will also be inescapable. In times like these, have your caretaker or family member know how you are feeling at every point of time. They will also be coached on how to take care of you by the surgery team.
If your entire pancreas has been removed, your doctor will have to prescribe insulin and enzyme supplements to you because they were being organically made in your pancreas earlier when it had been in a much better condition.
If there is the slightest change in your health during your downtime at home, please let your dear ones know so that after your doctor has been alerted, they can eliminate your predicament as soon as possible.
7. Risks and complications of a pancreas surgery
The unhidden fact is that half of the patients are likely to develop some kind of complication during the surgery or while recovering.
This segment of the blog will be unveiling some risks which may introduce themselves to a prospective pancreatic surgery patient.
It is always advised to talk about these risks with your doctor beforehand.
● Leakage of fluid from the pancreas after the surgery. Large amounts of leakage can cause an abscess which can further lead to infection or sepsis.
Fortunately, a Novartis-manufactured and FDA-approved drug known as Pasireotide is doing the rounds to rectify this problem. This drug blocks the secretions of digestive enzymes which tend to go into the abdominal cavity instead of the intestine.
● Exocrine pancreatic insufficiency (EPI) occurs when 90% of your pancreas is removed and when it is unable to make the digestive enzymes your body requires to absorb the nutrients from the food consumed.
● People who undergo a Whipple Procedure are 30 times more likely to develop EPI than those who undergo some other type of gastrointestinal surgery.
11% of people developed EPI after undergoing the distal pancreatectomy and it was a total of 5% who underwent central pancreatectomy.
The above statistics have been sourced from the Therapeutics and Clinical Risk Management journal which published the analyses in October 2019.
● Chest infections and blood clots are some of the other complications.
8. What you can expect ?
Before the procedure –
A general health check-up that will determine whether you are fit for a general anesthetic or not and how well your lungs and heart function will be conducted.Other tests that will be conducted include x-rays, blood tests and an extensive physical examination.
You will be asked to eat well and exercise aplenty. You may also be asked to take pancreatic enzyme supplements if you have pancreatic cancer since this condition tends to make one lose weight as cancer can affects the ability to digest food.
Your medical team may also ask you to take diabetes medication (if you have diabetes) and for thinning your blood.
During the operation –
In this four-to-seven hour operation, the patient will be unconscious throughout as they will be hooked to general anesthesia.
Don’t worry, their well-being will be constantly corroborated by an anesthesiologist.
After the procedure –
Expect to feel weak when waking up in the Intensive Care Unit (ICU). You shall stay there for a day or two.
While keeping a close eye on you, someone from the doctor’s team will give you antibiotics to prevent infections and injections to dodge any blood clots.
If your doctors are satisfied with the way you are recovering, you will be moved to a general surgical ward.
Pancreas surgery recovery time will vary from person to person.
9. How to choose a surgery centre ?
Keep the following points in mind when choosing the ideal surgery centre:
● Its reputation and whether it has a separate surgery wing as well as a celebrated team of specialists for treating pancreatic diseases
● Its postoperative programs and the benefits offered in them
● The duration of the hospital stay
● Its distance from your residence
● Whether this institution is recommended by a doctor you trust or if it aligns with your health insurance company’s policies.
It is also always helpful to converse with patients who have had pancreas surgery done in an institution which you think will be perfect for you.
10. Results of pancreas surgery
Pancreas surgery survival rate
For all stages of pancreatic cancer, the five-year survival rate is 7%. For pancreatic resection, the survival rate is 23 to 36 months.
11. Diet and nutrition after pancreas surgery
Water and squashes will make for the very first two liquids which you can consume post-surgery. Afterwards, more complex beverages such as tea and milk can be tried.
Remember that the time-frame for when normal eating and drinking can commence will vary from person to person.
Your dietician will also suggest that you start eating soft foods that can be chewed slowly.
Transplant Team
A liver transplant is an operation that involves the replacement of a patient's diseased liver with either a whole or partial healthy liver from a donor.

Dr. Abhijit Mane
Asst Consultant Liver & Multiorgan Transplant

Dr. Apurv Deshpande
Liver and Multi Organ Transplant

Dr. Manoj Raut
Consultant Liver Transplantation Anaesthesia & Critical Care
Transplant Team

Dr. Bipin Vibhute
Liver & Multiorgan Transplant Surgeon
A liver transplant is an operation that replaces a patient’s diseased liver with a whole or partial healthy operation that replaces.
Patient Reviews
Pravin Patole (Transplant Year: 2021)
Treatment : Liver Transplant
Saket Khadakkar (Transplant Year: 2021)
Treatment : Liver Transplant
Organ Donation
Why we should Donate Organs?
By Dr.Bipin Vibhute
The biggest donation in this world is Organ Donation, by which we can save multiple lives. To save someone’s life is the biggest thing in this world. Being a donor is like having superpowers. By donating organs you give hope or a chance of living to a person who has left all the hopes of surviving.
Even if a person dies, his organs are not dead. The organs of a dead person will be of no use after the body is burnt or buried. But these organs can save up to eight lives if we donate them. We all understand the importance of Organ Donation, but how many of us support and wish to donate our organs.
Question & Answers
What is the most common cause of cirrhosis in children
Out of the various organs in a human body, the liver performs some of the most important functions. This includes processing the good nutrients and passing it to the...
What should I eat if I have Nash?
NASH is a liver condition in which excess liver fat leads to inflammation. This will result in the development of liver scarring that will further lead to cirrhosis and...
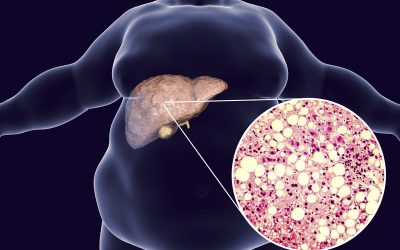
How does obesity lead to fatty liver disease?
Indeed, certain lifestyle choices have a major effect on your body, and that leads to further complications. One of the most common ones includes obesity, which results...
Blogs
Pancreas Transplant Cost in India: All You Need to Know
The cost of a pancreas transplant in India generally ranges from ₹7.95 lakhs to ₹15 lakhs, depending on the hospital, type of transplant, and individual patient needs....
Understanding Pancreatic Cancers
Pancreatic Cancer refers to the abnormal growth of malignant cells. It is characterized by the aberrant proliferation of malignant cells in the pancreas, which...
Healthy foods to eat after Pancreatic Transplant
Blog Category : Pancreatic TransplantA pancreas transplant is a surgery that involves the placement of a healthy pancreas of the donor into an individual (recipient)...