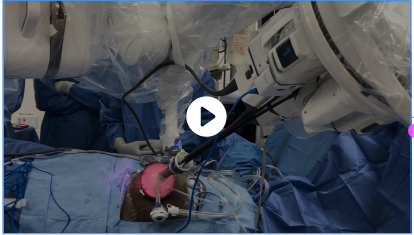
Liver Resection Surgery
By
Dr.Bipin Vibhute
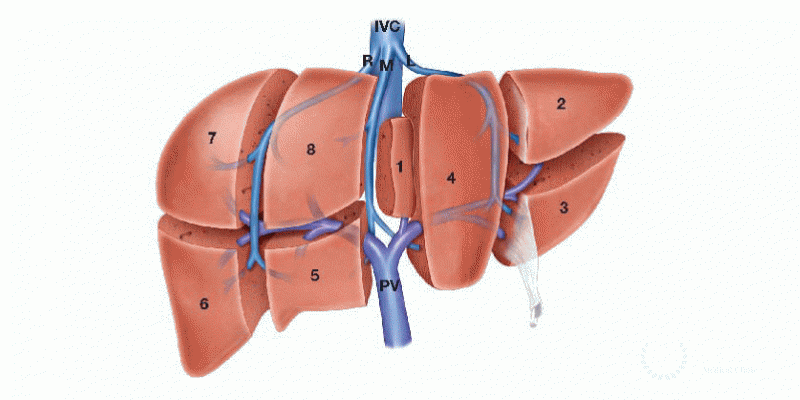
What is liver resection surgery?
Also known as a partial hepatectomy or a full hepatectomy, this is the surgical removal of a portion or all of the liver.
Complete liver resection is performed when a healthy liver is transplanted from a cadaveric donor to a recipient.
On the other hand, partial liver resection is performed with the help of a living donor in which they contribute only a piece of liver tissue.
Liver Resection Surgery Guide
You or someone you know may be in this condition. If this is so, invest your time in reading this blog that covers every aspect of this surgery.
1. Indications for hepatectomy
One should always know the symptoms of a disease they suspect they may have. And, the most conspicuous symptom of liver resection is the presence of various types of tumors in their liver.
Patients with liver cancer (Hepatocellular Cancer or HCC) who have one or two small tumors will be eligible for liver resection surgery.
A liver resection will be undertaken to treat:
Benign hepatic neoplasms such as-
● Hepatocellular adenoma
● Hepatic hemangioma
Focal nodular hyperplasia
And, malignant hepatic neoplasms such as:
● Metastases that arise from colorectal cancer
● Hepatocellular carcinoma
● Intrahepatic gallstones
● Parasitic cysts
2. Who might need a hepatectomy?
Individuals suffering from liver cancer who have the presence of one or two small tumors (3cm or less) without associated cirrhosis can undergo this surgery.
However, the number of patients who are eligible for this surgery is less because of the fear of developing liver failure post-surgery.
3. Purpose of the liver resection surgery
The sole purpose of a liver resection surgery is to remove any tumors or the appropriate surrounding liver tissue in the individual’s liver. Only a few patients undergo this operation because of the strict guidelines that depend on the tumors being small in size and low in number.
What all prospective patients should be well-aware of is that the normal, non-tumor portion of a liver, if removed, will grow back or regenerate, in a few weeks. However, a liver affected by cirrhosis will not grow back anytime soon.
Therefore, expect your surgeon to biopsy your non-tumor liver so that they can determine whether there is an existence of associated cirrhosis or not.
4. What is hepatectomy liver failure?
Patients bearing small tumors in their liver without associated cirrhosis can be selected to undergo liver resection. However, the rate of patients going through it is pretty low as there is a fear of liver failure post-surgery.
Also known as a post-hepatic-liver failure (PHLF) , it can occur when the remaining portion of the liver also starts to behave inadequately. The number of PHLF cases that have occurred are somewhere between 1.2% to 3.2%.
5. Hepatectomy failure causes
At first glance, one would wonder what could possibly go wrong with a liver resection surgery since its primary purpose was to make things right in an individual’s liver. However, the complications surrounding a hepatectomy are so grave and so many that the causes of hepatectomy failure can neither be discounted nor ignored.
These physical and physiological conditions may become contributing factors of hepatectomy failure:
● Diabetes
● Decreased immune function
● Hepatic steatosis
● Presence of lung disease (renal insufficiency)
● Advanced age
● Damage caused by some chemotherapy agents
● Pre-operative malnutrition
And, these are the factors that significantly impact a hepatectomy during a surgery:
● Blood loss
● Need for vena caval or some other vascular resection
Last but not least, these are some post-operative factors which can become the causes of PHLF:
● Post-operative hemorrhage
● Intra-abdominal infection
6. How is hepatectomy failure managed?
By a team of highly-experienced and well-educated team of surgeons or surgeon who initially and carefully chooses the patients who will benefit massively from the hepatectomy. Such surgeons should have prior experience of carrying out high-volume liver operations.
In the case of managing the hepatectomy, different techniques or strategies are used by various surgeons from several institutions.
For example, to treat jaundice in case of POHF, the surgeons will try and rule out the obstructive component and stay vigilant, overall. Or, in the case of suspected infection, early use of antibiotics will come in handy.
7. Types of hepatectomy
Call it types or call it techniques of hepatectomy. Either way, there are six in total and as a potential patient or a caregiver, you should know the most general information about each one.
1. Right hepatectomy: Also known as hemihepatectomy, this technique refers to the re-sectioning of the liver on the right side of Cantlie’s line ( an imaginary division dividing the liver into two planes) in the right side of the mechanical heart valve (MHV).
2. Left hepatectomy: One of the standard procedures of hepatectomy, it consists of three parts: hilar dissection of the left portal pedicle, mobilization of the left liver, and parenchymal dissection.
3. Left lateral hepatectomy: Also known as left lateral liver Sectionectomy, it is a surgical procedure in which the left lobe of the liver is removed. This even includes all the liver tissue left of the falciform ligament.
4. Extended right hepatectomy: Also known as trisegmentectomy, this surgical procedure becomes necessary when malignant tumors occupy a large part of the right lobe with extension into the medial segment of the left lobe.
5. External left hepatectomy: Such a technique is taken into consideration when large, strategically placed, left-sided and central hepatic lesions extend to involve the right anterior sectoral portal pedicular structures.
6. Segmental hepatectomy: This surgical technique involves the resection of one or more anatomic segments of the liver. And, the most common anatomic segments are right posterior sectionectomy, left lateral sectionectomy and caudate lobe resection.
If you are unable to comprehend the above medical terms, don’t scratch your head in confusion. Your surgeon or a senior member of their team will be able to explain each type to you in detail so that you will know what is to become of your liver during the hepatic resection surgery.
8. How is hepatectomy performed?
The more a prospective patient or their family knows, the better.
What needs to be kept in mind is that the liver resection surgery is not only considered major but also one that is seen as an ‘intervention’ of sorts. Consider it life-saving because it tries to restore the health of your liver that has now become inundated with a tumor or two.
With that being established, the surgeon will start with a bilateral sub costal incision, possibly with midline extension. A liver resection surgery may be anatomic (adhering to the limits of one or more functional segments of the liver as defined by the Couinaud classification) or non-anatomic meaning they could be irregular segments.
The reason why the latter approach is not preferred is because of the fear of bleeding and biliary fistula. However, it is often carried out successfully in many cases.
The anatomical approach is preferred universally as there is reduced risk of complications mentioned above.
9. Cost of hepatectomy
The cost of the heaptectomy will depend on a variety of factors that your surgeon will take into consideration before labeling a cost to a surgery that will significantly improve the quality of your life.
The following factors will be considered:
● The patient’s overall health and age
● How much of the liver has been compromised
● Damage to the tumor-free liver
The surgeon’s fees, the cost of the hospital stays and the medicines will also hike up the cost of the hepatectomy.
Worrying gets us nowhere. Therefore, if you are introduced to a financial coordinator at your chosen transplant centre, speak to them at length about your options.
Your health insurance should also be able to cover a portion of your operation.
10. Care after hepatectomy
As with any other surgery or transplant, we recommend having your caretaker or family member take genuine care of you.
Before you leave the transplant centre, the surgeon and the transplant team will monitor you 24/7.
Right after a hepatectomy, there are bound to be fluid and electrolyte imbalances as well as fluctuating liver function.
A sodium restriction and the controlled use of diuretic therapy will be recommended.
A thing to contemplate on is that when the liver is stressed, it produces lactate instead of metabolizing it. Therefore, non-lactose containing solutions will also be recommended after your operation.
11. Risks and complications from liver resection surgery
We have already explained that POHF is the most feared complication after a hepatectomy. But, there are other risk factors that surgeons and patients both must be wary of. They are:
● Bleeding
● Biliary fistula
● Atelectasis
● Pleural effusion
● Infections are comparatively rare but not uncommon.
12. How to choose a transplant centre
When choosing a transplant centre for hepatectomy, keep the following points in mind:
● Availability of supremely experienced medical practitioners and a team that will be in constant contact with you throughout the procedure
● Survival and biliary complication rate
● All the safety measures provided
● Postoperative support and amenities
● Availability of state-of-the-art medical facilities
Other than this, when choosing a transplant centre for hepatectomy, look out for its location and give thought to the cumulative cost of the surgery as well.
13. What you can expect?
Before the procedure
While your chosen surgeon will beseech you to stay healthier than you have ever been, they will also conduct many tests to gauge how bad the situation is. Some tests that will aid them in their diagnosis are:
● Physical examination
● Blood tests
● CT scan
● Ultrasound test
● MRI
● Angiograms
● Biopsy
During the procedure
As is known, clean towels will be placed on the patient’s face, along their sides and across their knees.
The anterior portions of the chest, the abdomen, and the lower extremities down to the knees will be scrubbed with betadine for 10 minutes. If the patient is allergic to iodine, hibiscrub will be used as an alternative.
Right after, two sterile towels will be used to pat the area dry. This area will then be smeared with iodine in alcohol. And, the draping process will involve side drapes, arm board drapes, top and bottom drapes, and a large steridrape.
After the procedure
After being taken to the Intensive Care Unit (ICU), the patient can expect to stay in the hospital for at least a few days(Usually 5 days). This surgery is a big deal and therefore, recovery will not only take time but also vary from person to person.
Apart from postoperative effects such as diarrhea, a feeling of fullness in the abdomen and weariness, the surgeon and the transplant team will constantly be on the lookout for any signs of complications such as bleeding or liver failure.
Your caregiver or family member can discuss pain management with the authorities concerned if you feel uncomfortable at any point.
When going home, you or the individual responsible for taking care of you will also be coached on how to keep your wound clean and uninfected.
14. Results after surgery
Hepatectomy survival rates
It’s important to disclose that the survival rates of a hepatectomy go up when after a partial liver resection surgery, liver function resumes normally or after a full hepatectomy, the transplanted liver starts functioning like normal.
Survival rates depend on the extent of liver cancer and the quality of liver function. In the last 1-2 years, the five-year survival rate has jumped from 35% to 50%.
15. Diet and nutrition after hepatectomy
Your diet should be well-supplied with nutritional balance and healthy eating habits. A Glycemic control should be established and precautions should be taken to not have your wound/incision infected.
When your stomach feels upset or you feel queasy, try eating low-fat and bland foods such as plain yoghurt, toast or boiled chicken. We don’t need to remind you that you must drink plenty of fluids because the nutritionist or the dietician from your transplant team will do so.
No matter what you do, abstain from gaining weight while recovering. Drinking alcohol after one month of surgery will be considered acceptable. However, if you have had a liver transplant, you must not think of consuming any alcoholic beverages.
16. Exercise tips for patients
The physiotherapist from your transplant team will suggest an array of exercises that will help you in breathing and regaining strength.
You will be advised to walk as it is considered a gentle exercise. Before you undertake any form of rigorous exercise, be sure to speak to your surgeon beforehand.
Transplant Team
A liver transplant is an operation that involves the replacement of a patient's diseased liver with either a whole or partial healthy liver from a donor.

Dr. Abhijit Mane
Asst Consultant Liver & Multiorgan Transplant

Dr. Apurv Deshpande
Liver and Multi Organ Transplant

Dr. Manoj Raut
Consultant Liver Transplantation Anaesthesia & Critical Care
Transplant Team

Dr. Bipin Vibhute
Liver & Multiorgan Transplant Surgeon
A liver transplant is an operation that replaces a patient’s diseased liver with a whole or partial healthy operation that replaces.
Organ Donation
Why we should Donate Organs?
By Dr.Bipin Vibhute
The biggest donation in this world is Organ Donation, by which we can save multiple lives. To save someone’s life is the biggest thing in this world. Being a donor is like having superpowers. By donating organs you give hope or a chance of living to a person who has left all the hopes of surviving.
Even if a person dies, his organs are not dead. The organs of a dead person will be of no use after the body is burnt or buried. But these organs can save up to eight lives if we donate them. We all understand the importance of Organ Donation, but how many of us support and wish to donate our organs.
Question & Answers
What is the most common cause of cirrhosis in children
Out of the various organs in a human body, the liver performs some of the most important functions. This includes processing the good nutrients and passing it to the...
What should I eat if I have Nash?
NASH is a liver condition in which excess liver fat leads to inflammation. This will result in the development of liver scarring that will further lead to cirrhosis and...
How does obesity lead to fatty liver disease?
Indeed, certain lifestyle choices have a major effect on your body, and that leads to further complications. One of the most common ones includes obesity, which results...
Blogs
Which Doctor Treats Fatty Liver? When to Consult a Liver Specialist
A hepatologist treats fatty liver disease. Know when abnormal liver tests need specialist care & get expert liver treatment in Pune before damage worsens.
Fatty Liver Grade 1, 2, and 3: What Each Stage Means and How It Is Treated
Fatty liver Grade 1 is reversible, Grade 3 risks cirrhosis. Know your stage, symptoms & best treatment. Expert liver care in Pune.
When Should You See a Doctor for Fatty Liver? Warning Signs You Should Not Ignore
Fatigue, belly pain, or jaundice? These could be fatty liver warning signs. See a liver specialist in Pune before damage gets worse.